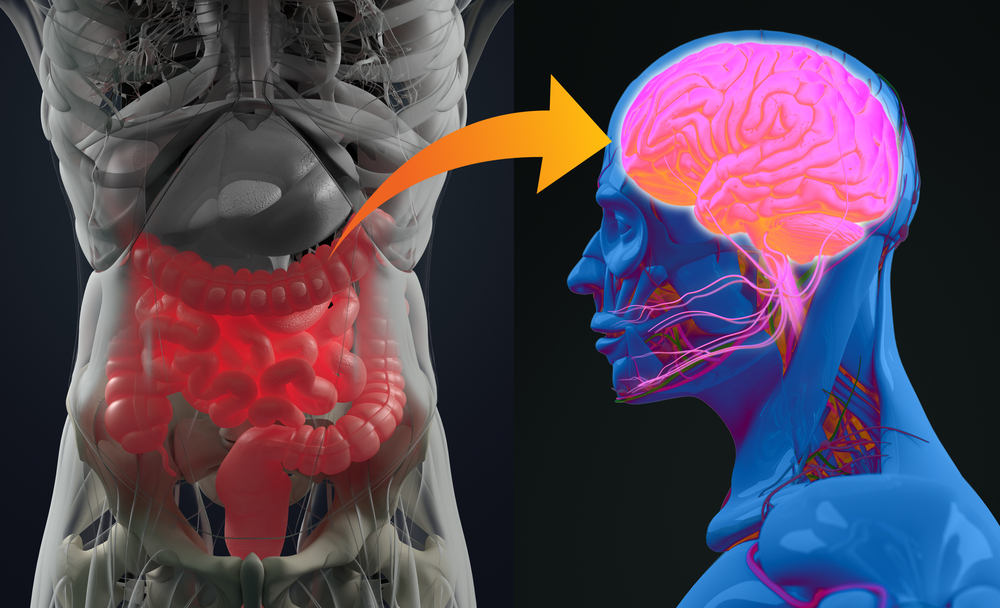
For decades, mental health treatment has focused almost entirely on the brain — medication, psychotherapy, and lifestyle changes aimed at improving mood, cognition, and resilience. But in recent years, science has been turning its attention further south, to the gut, and to a remarkable two-way communication system known as the gut–brain axis.
This connection has profound implications for how we understand — and potentially treat — mental health conditions, from anxiety and depression to bipolar disorder.
A Story That’s Turning Heads
On Australian Story this week, viewers met Jane, a woman whose severe, treatment-resistant bipolar disorder had controlled her life for years. After exhausting conventional therapies, Jane underwent a faecal microbiota transplant (FMT) — a procedure that transfers healthy gut bacteria from a donor into the patient’s intestines.
Important Caveat:
Astonishingly, Jane experienced long-term remission from her symptoms. While her story is extraordinary and offers hope to many, the program made it clear that FMT is still experimental for psychiatric use. The procedure is approved in Australia only for recurrent Clostridioides difficile infections, not for mental health conditions. Larger clinical trials, strict screening processes, and medical oversight will be essential before it can be considered a legitimate therapeutic option for mental health.
That said, Jane’s case adds weight to a growing body of research showing that gut health plays a significant role in mental wellbeing.
The Gut–Brain Axis: Why It Matters
The gut is often referred to as our “second brain” — and for good reason. It contains its own nervous system, the enteric nervous system, which communicates constantly with the brain via the vagus nerve and through chemical messengers.
But one of the most fascinating players in this conversation is the gut microbiome — the trillions of bacteria, fungi, and other microorganisms living in our digestive tract. These microbes produce neurotransmitters like serotonin, dopamine, and gamma-aminobutyric acid (GABA), all of which affect mood and mental clarity. In fact, about 90% of the body’s serotonin is made in the gut .
When the gut microbiome is balanced and diverse, it can promote emotional stability, better stress regulation, and even sharper thinking. But when it’s disrupted — through poor diet, chronic stress, illness, or antibiotic overuse — it may contribute to mood disorders, anxiety, and even cognitive decline.
Diet and Probiotics: Everyday Tools for Mental Wellness
The Australian Story segment didn’t just focus on FMT — it also highlighted practical, everyday strategies for maintaining gut health, including a nutrient-rich diet and the use of probiotics.
A diet rich in plant-based fibres, whole grains, fruits, vegetables, and fermented foods (like yoghurt, sauerkraut, and kefir) feeds beneficial gut bacteria and supports a healthy microbiome. Probiotics — live microorganisms that can confer health benefits — can help restore balance, especially after gut-disrupting events like illness or antibiotic use.
Where NutriKane R Fits In

This is where NutriKane R comes into the picture. As one of the linchpin products in the NutriKane range, it was scientifically formulated to:
- Promote regularity
- Support microbiome diversity
- Stimulate the intestinal tract
- Provide a natural source of dietary polyphenols and resistant starch
Unlike experimental therapies like FMT, NutriKane R is already available, all natural, Australian made, and backed by research. It’s not a replacement for medical care, but it can be a powerful adjunctive therapy — something you can integrate into daily life to improve gut health, which in turn may benefit your mental wellbeing.
The Bigger Picture: Mental Health and Society
One of the most striking statistics from the program was that mental health issues are costing the Australian community over $70 billion every year in healthcare, lost productivity, and social support.
If we can find ways to address root causes — or even contributing factors — of mental illness, the ripple effects could be enormous. Supporting the gut–brain connection is one promising avenue, and unlike some high-tech interventions, it’s one that can start with something as simple as changing what’s on your plate.
Looking Ahead
While FMT for psychiatric conditions is still in the research phase, the science supporting the gut–brain axis is strong and growing stronger. Whether it’s through fibre-rich foods, probiotic supplements, fermented foods, or scientifically formulated products like NutriKane R, the message is clear: a healthy gut is a foundation for a healthy mind.
In the future, we may see gut-based therapies become a standard part of mental health care. For now, the simplest, safest, and most accessible step you can take is to nourish your microbiome every day. Your mind just might thank you for it.
Feel free to visit our website www.nutrikane.com.au for further information or give us a call!
References:
- Mayer, E. A., et al. (2015). “Gut/brain axis and the microbiota.” Journal of Clinical Investigation, 125(3), 926–938.
- Foster, J. A., & McVey Neufeld, K. A. (2013). “Gut–brain axis: how the microbiome influences anxiety and depression.” Trends in Neurosciences, 36(5), 305–312.
- Collins, S. M., Surette, M., & Bercik, P. (2012). “The interplay between the intestinal microbiota and the brain.” Nature Reviews Microbiology, 10(11), 735–742.